HIPAA EDI Process Flow: From Eligibility to Claims Payment with Controls That Auditors Love


The journey from insurance eligibility inquiry to claims payment is a lifeline for healthcare payers. Yet it’s a labyrinth of rules, formats, security requirements, and compliance demands. As a team that works daily with the intricacies of HIPAA EDI data, we’ve seen how mastering the process—and building in the right controls—transforms chaos into clarity, reduces time to cash, and keeps auditors happy. This guide will take you behind the scenes through each step of HIPAA EDI process flow, highlight what truly matters to compliance officers and end users, and show how granular controls and real-time visibility set the bar for modern insurance operations.
What Is HIPAA EDI? A Unified Language for Healthcare Transactions
HIPAA EDI refers to a set of federally mandated standards (especially X12 formats) for electronic exchange of insurance data among payers, providers, and third parties. For us in the payer world—whether health, dental, or vision—embracing these standards is foundational. Eligibility inquiries (270/271), claims (837), payments (835), acknowledgements (999, TA1), and status inquiries (276/277) all move as precisely structured EDI files. The payoff: we trade re-keying and manual audits for automation, rapid verification, and a digital trail of every action.
A Step-by-Step Look: The EDI Process Flow from Eligibility to Payment
- Eligibility Verification (EDI 270/271)
Everything starts with understanding the member’s coverage. Providers or partners submit an EDI 270 request to a payer—our systems validate and translate the request instantly, parsing out subscriber and dependent data regardless of incoming format (EDI, Excel/CSV, XML, or custom layouts). An EDI 271 response returns the member’s coverage, active plan details, co-pays, and deductible data.- Why strong controls matter: Automated validation and field mapping catch incomplete or malformed requests before they even hit your core system. Role-based activity logs and real-time alerts reduce time-to-resolution and arm auditors with every lookup and correction made on file.
- What we’ve learned: End users thrive when they get real-time status (covered/not covered), with instant analytics on eligibility trends—no more help desk bottlenecks or IT fire drills.
- Claims Intake, Translation, and Submission (EDI 837)
Once services are rendered, providers prepare claims which arrive in a variety of shapes and sizes. Our daily challenge is to turn all that data (from ancient positional files to sleek API feeds) into gold-standard EDI 837 files. This step relies on EDI translators, custom field validations, and payer-specific rulesets that enforce compliance before the claim even leaves your side.- Controls auditors love: Before a single claim is submitted, enforce SNIP Levels 1-7 validation to catch typos, missing codes, or logic errors. Every file version, edit, and submission should be logged with user and timestamp for a seamless audit trail.
- The reality: Strong pre-submission controls reduce downstream rejections, while unified dashboards replace manual ‘status chasing’ for operations staff.
- Transmission, Acknowledgement, and Tracking (TA1, 999, 277CA)
Now it’s time to send the EDI 837 file to a clearinghouse or payer. You’ll get back a TA1 (for envelope structure) and a 999 (for X12 compliance) followed by a 277CA (offering a first pass at acceptance/rejection). Each response carries clues about data issues or downstream processing status.- Best practices: Log every submission, response, and error with immutable, timestamped records. Set up automated alerts for rejected files or missing acknowledgments so fixes happen within SLA windows. Live dashboards empower teams to prioritize remediation and streamline compliance review.
- Claims Adjudication and Status Inquiry (EDI 276/277)
Following submission, the payer reviews and adjudicates the claim. Providers may initiate a 276 status inquiry, and our system responds with a 277 status file, detailing whether the claim is still in process, denied, or paid. Forward-thinking teams use automated exception routing so tricky cases get human eyes fast, not days after a file sits in limbo.
- Remittance Advice & Payment (EDI 835)
Finally, after adjudication, payers issue an EDI 835 remittance file explaining payments, denials, and adjustments. The goal: reconcile every penny and every claim line to its originating EDI 837 and status history. Audit trails that span the full journey (from eligibility to payment) are invaluable for both compliance and revenue cycle management.

Compliance and Audit Controls: What Actually Impresses Auditors
There’s no shortcut when it comes to HIPAA compliance, especially with EDI. We’ve worked alongside audit teams and compliance officers, so we know what stands up during reviews. Here are the controls that move the needle for insurers and TPAs:
- Real-Time Validation: Automatically detect syntax and logic errors, stopping non-compliant files at the source. Configurable by payer and transaction type.
- Immutable Audit Trails: Every edit, view, and submission is logged with who, when, and what changed, helping fulfill HIPAA, SOC-1, and SOC-2 demands.
- Automated Alerts and Exception Management: Instant, role-based alerts for file rejection, data exceptions, or SLA risk. SLAs are not just monitored but are actionable, closing the loop on compliance and performance.
- Role-Based Access and Security: Leverage multi-factor authentication, strong encryption, and strict control over who can view, edit, or approve files. This aligns with the strictest interpretations of HIPAA and modern IT best practices.
- Comprehensive Reconciliation: Trace every dollar and claim line from submission to adjudication, with seamless linkage of eligibility checks, claim files, status updates, and payment records.
Metrics That Matter: How Automation Changes the Numbers
For technology leaders and operations teams, we know metrics drive decision-making. Here’s what we’ve consistently observed with robust, automated EDI controls:
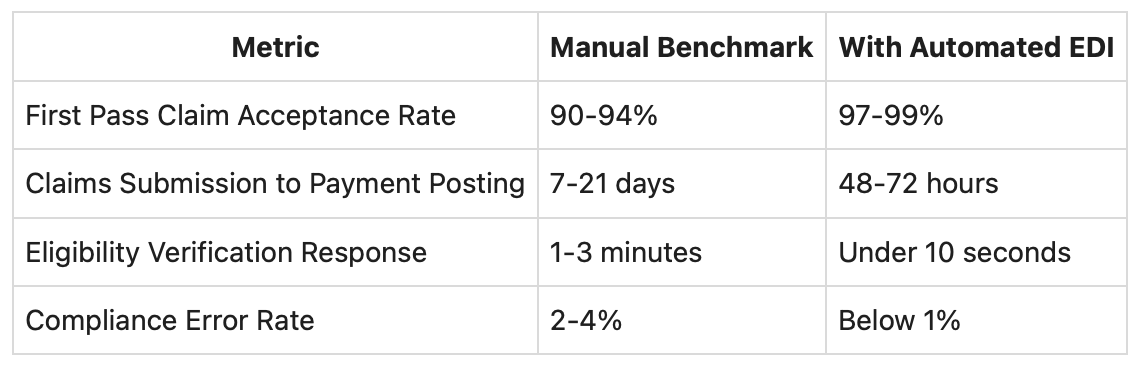
These numbers mean happier members, faster revenue, and dramatically less stress at audit time. For a broader view on KPIs and driving EDI outcomes, see our guide to the KPIs that drive EDI success in health insurance.
EDI Sumo’s Perspective: Making Data Available, Usable, and Audit-Ready
At EDI Sumo, we don’t just plug a tool into your stack. We work with payers to navigate the unique complexity of every data feed, file, and workflow, turning EDI from a black box into an accessible, auditable, and proactive foundation for your operations.
- Support for all major formats (EDI, CSV, XML, APIs) so you never get stuck retrofitting.
- Real-time dashboards that empower claims, enrollment, and customer service teams.
- Enterprise-grade audit trails and compliance reporting to keep you ahead of auditors, not scrambling after them.
- End-to-end integration, from intake and eligibility to payment posting, so you never lose sight of the full process.
- Enterprise security, including advanced encryption, MFA, and fine-grained user controls, protecting both privacy and internal governance. More details are available in our Trust Center.
Navigating Forward: Tips for Payers, Enrollment, and Claims Directors
- Map every input: Don’t settle for a tool that only accepts one format. Multi-format translation and robust mapping let your operations scale with partners and vendors of any size or legacy system.
- Turn audit readiness into an ongoing process: Ensure controls, logs, and reports aren’t a last-minute scramble—they should be part of daily operations.
- Break data out of silos: Data should be visible and usable across claims, enrollments, and service teams, not isolated inside IT or hidden in flat files.
- Prioritize proactive alerts: The best issue to fix is the one you solve before a denial, SLA miss, or audit finding. Empower your team with real-time notifications and dashboards.
Stop Dreading the Audit. Start Empowering Your Team.
If you want to see how data-driven, real-time auditability, and end-user empowerment can work in your operation, see more about EDI Sumo at www.edisumo.com. We help health, dental, and vision payers take the guesswork out of EDI, stay ahead of HIPAA, and remove data headaches from IT.


.png)






.png)

.png)


.png)
