Year-End HIPAA Readiness: 12 EDI Control Tests to Pass SOC-2 and Internal Audit Reviews


With year-end audit season approaching, every healthcare payer faces the pressure of showing ironclad HIPAA readiness and passing tough SOC-2 and internal reviews. At EDI Sumo, we live in the intersection of regulatory compliance and seamless EDI operations. Our work standardizing enrollment, eligibility (834), and claims (837) data for payers—including vision, dental, and health—means we see firsthand what separates audit success from an expensive, stressful remediation scramble.
EDI 834 Transactions Explained: The Foundation of Enrollment Data
The EDI 834 is the industry-standard format for transmitting benefits enrollment and maintenance data between employers, insurers, and vendors. Think of it as the DNA of healthcare eligibility—without accurate 834 files, member enrollments fall apart, coverage lapses, and downstream claims get rejected.
- Contents: Demographic info (name, DOB, ID), policy numbers, coverage dates, plan details, subscriber/dependent relationships, and qualifying life events.
- Key Compliance Risks: Missing/duplicate records, incorrect effective dates, formatting errors, or PHI exposure during file transfers.
- Audit Control: We recommend automated receipt validation, schema checks, and full audit trails for every EDI 834 transaction. This not only aligns with HIPAA Data Integrity standards, but also supports SOC-2 Processing Integrity criteria.
The move toward real-time eligibility and automated enrollment updates makes the quality and monitoring of 834 transactions more critical than ever.

What Are SNIP Levels? A Practical Guide for Payers and Providers
To ensure your EDI files are truly compliant—especially enrollment (834) and claims (837)—you need more than a file that simply "loads". The Workgroup for Electronic Data Interchange (WEDI) developed SNIP (Strategic National Implementation Process) validation levels as an industry benchmark for EDI testing:
- Level 1: Syntax integrity. Validates basic structure, segment counts, mandatory elements.
- Level 2: Required data elements. Looks for required loops, correct qualifiers, ID lengths.
- Level 3: Balancing. Ensures counts, control numbers, financial data align end-to-end.
- Level 4-7: Code sets, situational rules, gender/age checks, payer-specific logic, and adjunct validation.
Achieving SNIP Level 7 validation is considered a gold standard, but most payers at least demand passing Levels 1-3 for all inbound and outbound EDI. Failing SNIP validations leads to downstream data quality issues, rejected claims, and a big audit red flag. For practical strategies on implementing SNIP validation, we shared detailed steps in this SNIP guide.
EDI 999 vs. 277: What’s the Difference and Why It Matters for Payers
When we talk about EDI audit readiness, knowing your acknowledgment files is essential. SOC-2 and HIPAA both require proof that your systems confirm receipt (or rejection) of files, providing a traceable data handshake at every step.
- EDI 999 (Functional Acknowledgment): Sends back generic receipt status for any X12 file, confirming if the incoming file was received and is structurally valid.
- EDI 277CA (Claim Acknowledgment): Offers more granular feedback, especially for claims transactions (837). The 277CA specifies which claims within the batch passed or failed validation, making it crucial for claims traceability and error management.
Payers should monitor not just that acknowledgments are sent, but that they're timely and correctly linked to the original files. Consistent gaps or delays in 999/277CA delivery are a major cause of audit findings and can expose you to compliance risk.
For a deeper dive on the difference and downstream implications, see our blog on EDI Health Insurance Basics.
EDI 837 Claims Transactions: Why Accuracy and Speed Matter for Payers
The EDI 837 is the backbone of healthcare claims processing, covering professional (837P), institutional (837I), and dental (837D) transactions. For payers, accurate and fast claims handling directly impacts revenue cycles, member satisfaction, provider relations, and—most importantly—regulatory compliance.
Why are 837 controls so critical for audits?
- Claims edits and rejection handling: Audit teams want assurance that invalid or out-of-balance claims are flagged and returned, not simply loaded as errors into back-end systems.
- Acknowledgments (277CA): The traceability of claim status—including when and why a claim was rejected or corrected—is essential for passing both HIPAA and SOC-2 audits.
- Integration and visibility: Siloed or delayed claims files can trigger denied payments, member grievances, and audit citations. Our unified dashboard approach (with real-time reporting and alerts) helps stakeholders access accurate claims data when it matters most.
To fully understand the impact of 837 claims accuracy and speed, explore our practical breakdown: Turning EDI Transaction Data Into Actionable Insights.
12 EDI Control Tests for Audit-Ready HIPAA and SOC-2 Compliance
We compiled the following practical control tests based on both published standards and on-the-ground experience with payer audit teams. Use this as your daily operational checklist and year-end audit roadmap:
- File Receipt and Data Integrity Validation
Ensure every file (834, 837, etc.) is received, logged, and validated for correct record counts. Automate checksums and structure analysis to flag missing/corrupt data. - Access Control and Segregation of Duties
Enforce role-based access. Quarterly reviews to deprovision ex-users and segregate sensitive processing duties. - Full Audit Trail and Monitoring
Log every EDI file event, from receipt to processing and acknowledgment. Retain logs for at least six years to meet audit discovery requests. - HIPAA-Compliant Transmission Security
Require TLS 1.2+ encryption or higher (SFTP, AS2, etc.) for all data in transit and at rest. Review and update encryption keys and ciphers annually. - SNIP-Level and Custom Validation
Automate SNIP Levels 1-7 and overlay payer-specific business rules for every file. Reject or quarantine failed files with clear feedback loops. - Automated Acknowledgment Process (999/277CA)
Confirm acknowledgments for every EDI file (both inbound and outbound) and track delivery status in real time. - Business Associate Agreements (BAAs) Review
Confirm that BAAs with all third-party vendors are signed, updated, and reviewed annually. Perform vendor risk assessments regularly. - Backup and Disaster Recovery Simulation
Perform periodic restore and failover tests. Document and measure your actual RTO and RPO against contract or policy requirements. - Change and Mapping Management
Log every EDI map or code change with peer review and version history. Certify mappings before production release to prevent data transformation errors. - PHI Redaction and Masking
Test your redaction process on all test and troubleshooting data. Conduct random spot checks for PHI leakage in non-production environments. - Incident Response Plans for EDI
Simulate an actual EDI exception—such as corrupted file or unauthorized access—at least once a year. Update playbooks with lessons learned. - Performance and Exceptions Monitoring
Track metrics like processing times, exception rates, and year-over-year improvement. Provide structured evidence during audits or reviews.

Operationalizing the Checklist: How to Stay Audit-Ready All Year
- Audit assessments should be scheduled early (by December 1) to identify and remediate possible control gaps before year-end.
- Unified audit trails: Use tools that centrally log every record touch, validation event, and exception for fast evidence gathering.
- Formal documentation: Store structured evidence of each control test—auditors seek clear mapping to both HIPAA and SOC-2 requirements.
- Continuous team education: Regulatory standards and audit guidance change. Train your operations and IT teams regularly to shorten the learning curve at audit time.
Summary Table: EDI Control Tests and Their Regulatory Mapping
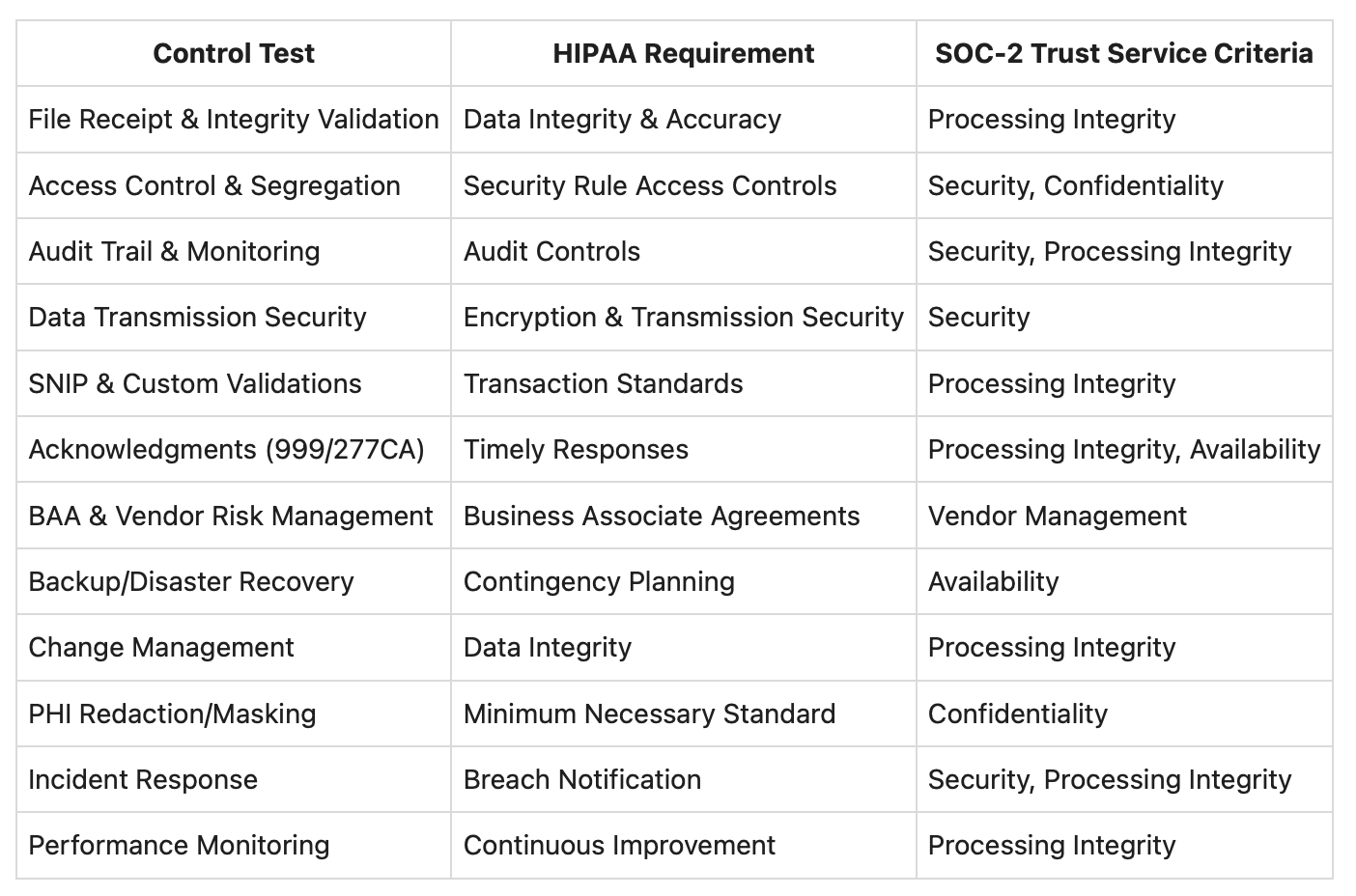
Conclusion: Don't Let EDI Controls Be Your Audit Weak Link
If your team wants to reduce audit stress, improve EDI data quality, and gain real-time control over enrollment and claims, see how we help leading payers stay ready for anything. Contact us to schedule a demo.


.png)






.png)

.png)


.png)
